Thrombophlebitis
Thrombophlebitis is a blood clot that forms in a vein in the body. Deep thrombophlebitis, or deep vein thrombosis, in particular must be treated quickly, as it can cause a pulmonary embolism. Learn more about thrombophlebitis and how to treat it.What is thrombophlebitis?
The word “thrombophlebitis” comes from two roots: thrombus, which means clot, and phlebitis, which means vein inflammation.
Superficial thrombophlebitis is therefore an inflammation of the superficial veins (those at the surface of the skin), which is generally associated with varicose veins or the insertion of needles . This condition has few risks of complications but shouldn’t be ignored, as it could lead to deep thrombophlebitis, which is a more serious problem that results in blood clots in the deep veins. A clot can then detach and travel through the circulatory system and become lodged in another part of the body. If the clot obstructs a pulmonary artery, this is called a pulmonary embolism. This blockage has serious consequences for the heart and lungs and can even cause death.
You need to know the symptoms and risk factors of thrombophlebitis so that you can act as quickly as possible.
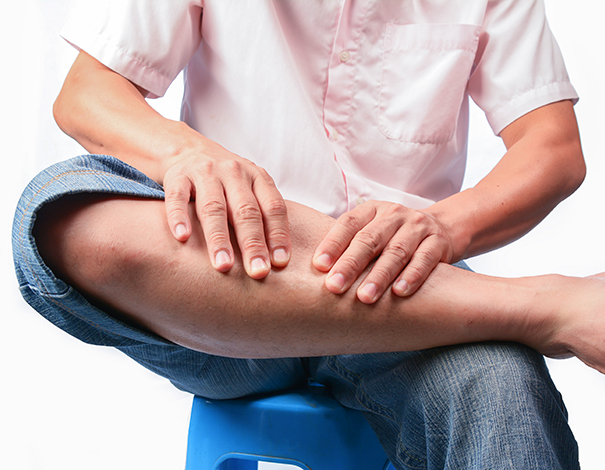
Thrombophlebitis symptoms
In the majority of cases, deep thrombophlebitis appears in a vein of the legs and particularly in the calf. Getting calf pain when you flex your foot with a straight leg is a possible symptom of this disease. Although more rare, phlebitis can also occur in a vein in the arm. Thrombophlebitis can have other signs and symptoms:
- pain or sensitivity in the leg
- swelling in the leg
- redness or discolouration of the skin of the leg
- skin that is warm to the touch
- skin that becomes taught
- fever
If you notice these symptoms, consult a doctor right away to prevent the risk of a pulmonary embolism. You’ll have to go to the emergency room for immediate care.
Deep thrombophlebitis may not cause any symptoms, which happens in about half of patients. You therefore need to be able to recognize the symptoms of a pulmonary embolism: shortness of breath, fast heart rate, chest pain, coughing, and coughing up blood. These symptoms require emergency medical care.
What are the main risk factors of thrombophlebitis?
The following factors increase the risk of thrombophlebitis:
- history of varicose veins or thrombosis (a blood clot in a vein or artery)
- family history of thrombophlebitis
- lying down, standing or sitting for extended periods (such as flying or after major surgery)
- obesity
- leg injuries or fractures
- pregnancy
- ulcerative colitis (a bowel disease) and other inflammatory diseases
- chronic heart failure
- cancer
- some surgical procedures
- smoking
- age
Women over 35 who take oral contraceptives, especially women with other risk factors, have a greater risk of developing thrombophlebitis.
How to prevent thrombophlebitis
Here are some tips to prevent clots:
- Avoid sitting, standing or lying down for an extended period. Change positions often to keep blood from pooling in your legs.
- Exercise regularly to improve your blood flow. It’s recommended that you do 30 minutes of moderate physical activity every day.
- Maintain a healthy weight. Obesity is a risk factor.
- Don’t smoke, and avoid exposure to second-hand smoke. If you’re having trouble quitting, don't hesitate to ask your pharmacist or doctor for help. They can make recommendations to help you stop.
- If you have varicose veins, wear compression socks. These socks compress the leg to force blood to return to the heart.
- On a long flight, stand up and walk around a bit every hour. You can also do stretching exercises in your seat. Remember to stay hydrated and avoid drinking alcohol during the flight. See your pharmacist for more tips about air travel.
How is thrombophlebitis diagnosed?
To diagnose thrombophlebitis, your doctor will start by checking your medical history and examining you. A physical exam is often inconclusive, and your doctor will probably order other tests (blood tests, ultrasound) to confirm that you indeed have a blood clot.
If your doctor finds a blood clot in a deep vein, you may have to be admitted to hospital.
Thrombophlebitis treatment
The main goal of treatment is to remove the blood clot and prevent a pulmonary embolism. If required, you may also be treated for chronic venous insufficiency, as this condition can sometimes lead to a clot and become a longer term complication of deep thrombophlebitis. A symptom of venous insufficiency is swelling and dilation of the superficial leg veins.
Anticoagulants
In the hospital, you will be given a subcutaneous or intravenous anticoagulant called heparin, which thins the blood and eliminates the clot.
When you start your treatment, you may also be prescribed another anticoagulant called warfarin. This medication is taken orally, and you’ll need to get a number of blood tests so that your dose can be adjusted. Warfarin treatment must be monitored closely. It’s important that you follow the recommendations of your doctor and pharmacist when taking warfarin. If your dose is too low, your blood will be thicker, and you risk getting a new clot. If your dose is too high, your blood will be too thin, and you’ll be more at risk of bleeding. This is why you must go to your appointments and get your ordered blood tests so that your warfarin dose can be adjusted accordingly. This dose varies from person to person and varies over time for the same person.
Other oral anticoagulants are now available on the market and can be prescribed instead of warfarin. Their benefits are that they don't require regular blood tests, and they’re effective from the start of treatment.
Your medication will depend on your personal characteristics and preferences. No matter what drug your doctor prescribes, your treatment duration will vary depending on your condition and the cause of your thrombophlebitis. You may have to take the medication for a few months to a few years.
A good understanding of your drug regimen will let you take full advantage of your treatment and minimize the risks. Have questions? Don’t hesitate to talk to your pharmacist or doctor. Ask them to explain anything you don’t fully understand. You can also ask a family member to go with you to help you understand and remember what your health care professional explained.
Compression socks
Along with anticoagulants, compression socks are generally recommended to promote blood flow to the heart and prevent another clot. Get more information from your pharmacist or your doctor.
Your health is important. Talk about it!
You must notify any health care professional you consult that you’re taking a blood thinner. You should also wear a medical ID bracelet that says “anticoagulant.” Warfarin and other anticoagulants can interact in a number of ways with some prescription and over-the-counter drugs and with a number of natural health products and foods. Always check with your pharmacist about whether you can take a certain drug or natural health product. Also check about interactions with food.
The pharmacy services presented in this section are offered by pharmacist owners who are affiliated with Uniprix. The pharmacists are solely responsible for the professional activities carried out during the practice of pharmacy. These services are offered in participating pharmacies only. Certain fees and conditions may apply.
* The information contained herein is provided for informational purposes only and is not intended to provide complete information on the subject matter or to replace the advice of a health professional. This information does not constitute medical consultation, diagnosis or opinion and should not be interpreted as such. Please consult your health care provider if you have any questions about your health, medications or treatment.
